Are IoT based ventilators promising or impractical?
Reading time 7 mins
Key Points
- COVID-19 highlighted gaps in healthcare infrastructure that technology can help to fill
- ‘Smart’ breathing machines could help to improve patient outcomes while reducing the workload of medical and nursing staff
- The longer that patients stay on a ventilator, the greater the risks become
- Pressure Support Ventilation (PSV) is one of the most commonly used modalities on ventilators in intensive care units. It requires clinicians to set the target pressure, monitor/adjust it regularly, and wean patients off it slowly
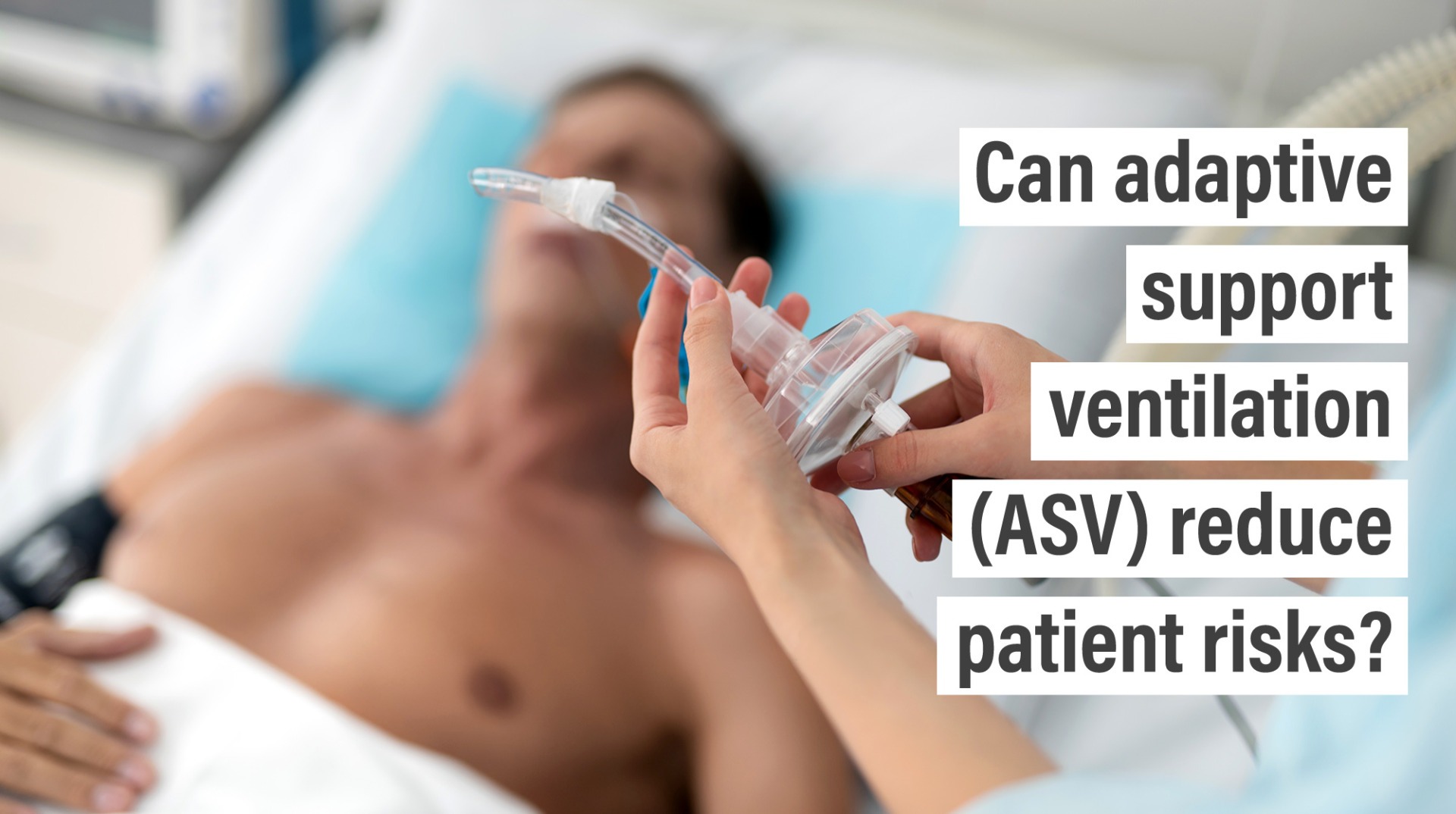
- Adaptive Support Ventilation (ASV) allows for personalised, responsive, and automated treatment and reduces some of the risks associated with PSV
- ASV isn’t being used by a wide range of clinicians, so its scope isn’t fully understood
Is your business ready to harness the potential of IoT? Our expert team can help design and implement bespoke IoT solutions. Reach out to us now to kick-start your IoT journey.
Ben Mazur
Managing Director
I hope you enjoy reading this post.
If you would like us to develop your next product for you, click here
The things we do instinctively are the ones we take the most for granted. Breathing most likely tops the list for many of us. The Corona Virus highlighted how the supply of, and access to, ventilators aren’t things we can take for granted. At the same time, it revealed gaps in healthcare infrastructure worldwide (e.g. who do doctors and healthcare workers get support from?) that technology such as IoT-based ventilators could help to fill.
A ventilator is a machine that helps you to breathe if you can’t do it on your own by pumping oxygen into your airway. Aside from COVID, there’s a large number of illnesses that cause people to have difficulty breathing. These include asthma, cardiac arrest, loss of consciousness, drug overdose, pneumonia, acute respiratory distress syndrome (ARDS), and surgery.
With many hospitals and healthcare facilities overburdened, would smart medical devices lighten the load or misdirect it?
What is the promise of ‘smart’ breathing machines?
Because ventilators are primarily used in hospital settings, they require a doctor or respiratory therapist to control how much oxygen the ventilator pushes into your lungs. Additional medical equipment to monitor how you’re doing overall (e.g. heart rate, blood pressure, oxygen saturation) are also likely to be used. The risks of being on a ventilator increase the longer you stay on one and can include the following:
- Infection, e.g. pneumonia or sinus infection from germs that accumulate in the breathing tube
- Irritation
- The breathing tube can damage your voicebox and lead to vocal cord issues
- Pulmonary oedema can occur if the air sacs in the lungs fill up with liquid
- Increased risk of blood clots due to lying down in the same position for too long
- Possible side effects such as sedation-related delirium as a result of the medication given (e.g. painkillers or sedatives) to keep you comfortable
Pressure Support Ventilation (PSV) is one of the most modalities used in intensive care units [1]. The ventilator provides assistance when the patient initiates a breathing effort. When the inhalation reaches a certain threshold level, the cycle to exhalation occurs.
- Clinicians set the target pressure
- This pressure needs to be monitored and adjusted regularly
- Patients need to be gradually weaned off the ventilator machine – requiring the clinician to reduce the pressure hourly
IoT stands for the Internet of Things. It refers to the network created when physical objects are embedded with sensors, software, and other technologies that allow them to connect to and with each other over the internet. The promise of IoT-based ventilators in a healthcare context is two-fold: improve patient outcomes while reducing the burden on medical staff and healthcare providers [2]. ‘Intelligent ventilator technology’:
- Allows lung treatment to be personalised by studying a patient’s condition and suggesting optimal clinical targets
- Allows for online, automated adjustments in real-time to respond to alterations in a patient’s needs
- Supports the optimal mechanics of ventilation for most patients
- Shortens the patient’s ventilation days
- Reduces morbidity rates
- Reduces weaning time
- Reduces medical and nursing staff workload as there’s less need for them to monitor and make changes to the ventilator pressure settings constantly
The pros and cons of IoT-based ventilators
A company at the forefront of this field, Hamilton Medical, has developed a range of ventilator technologies, with their adaptive support ventilation® (ASV) solution taking the lead. Their medical ventilation devices deliver on the promises outlined above – particularly regarding the ability to adapt to a patient’s changing needs. ASV automatically employs lung protective strategies to minimise complications and maximise positive patient outcomes.
The biggest drawback is that ASV is a mode unique to Hamilton Medical ventilators. This limits the number of clinicians using it; therefore, its scope isn’t universally understood [3]. In addition, smart modes undermine the position of respiratory therapists as the device can make changes (e.g. rate of respiration and pressure) autonomously and in the absence of a professional. Furthermore, this modality can be a contraindication for obese patients, those who have had cardiothoracic surgery, or people with restrictive lung disease [4].
Should we be ready to breathe a sigh of relief?
While the promise of IoT-based ventilators certainly isn’t an empty one, the lack of ASV modalities other than that developed by Hamilton Medical means that the jury is still out. Then there’s the risk to patients using medical IoT devices with automated features that don’t necessarily require a medical professional to be on standby at all times…Do we want ventilators to be in that category?
That said, this also highlights an area for further Research and Development, which is at the heart of everything we do – especially when IoT is involved. We recently wrote a post on how wearables can improve the administration of healthcare, and would be interested to see how these could apply in the context of ventilators. We’re not medical practitioners or respiration specialists, so we look forward to exploring this subject further and collaborating with industry experts along the way.
What’s your take on intelligent ventilator technology? Get in touch and share your thoughts – we’d love to hear them!
Comments
- Aguirre-Bermeo, H., & Mancebo, J. (2016, April). Pressure support ventilation. Oxford Academic. https://academic.oup.com/book/35534/chapter-abstract/305797711?redirectedFrom=fulltext
- HealthManagement.org. (2022, November 18). Intelligent Ventilation in the ICU: Technology Improving Patient Outcomes. HealthManagement. https://healthmanagement.org/c/icu/issuearticle/intelligent-ventilation-in-the-icu-technology-improving-patient-outcomes-1
- Journal of Mechanical Ventilation. (2022, September 17). Adaptive Support Ventilation (ASV). Beneficial or not? https://www.journalmechanicalventilation.com/abstract-adaptive-support-ventilation-asv-beneficial-or-not/
- Titus, A., & Sanghavi, D. (2020, August 19). Adaptive Support Ventilation. Europe PMC. https://europepmc.org/article/NBK/nbk560652
We love to talk about new ideas
Do you have an idea? Book a consultation with an expert - it's free, it's confidential and there are no obligations.
+44(0)117 329 3420
[email protected]
Ignitec Technology Centre
1 The Powerhouse
Great Park Road
Bradley Stoke
Bristol
BS32 4RU



0 Comments